How Many Types of Stem Cell Collection Are There? Where Can They Be Collected, and How Do They Differ?
How Many Types of Stem Cell Collection Are There? Where Can They Be Collected, and How Do They Differ?
Advancements in stem cell isolation and storage technologies have significantly expanded the potential applications of stem cells. Over the past decade, many people have become increasingly familiar with the concept of stem cells—whether regarding where they can be collected, which source is most suitable, or which diseases they can treat. This article provides an in-depth overview of the different sources of stem cells and their key characteristics.

How Many Types of Stem Cells Are There?
Currently, several types of stem cells are known and studied in medical science.[1,2,3,4] In clinical practice, stem cells are most commonly classified according to their cellular properties. Broadly, they can be divided into two main categories:
Hematopoietic Stem Cells This type of stem cell can self-renew and differentiate into only blood-related cells, such as red blood cells, white blood cells, and platelets. Consequently, their clinical use is primarily focused on hematological diseases. In some cases, hematopoietic stem cells have also been explored for non-hematological conditions, with the expectation that therapeutic benefits may arise from the growth factors or signaling molecules they produce. However, such applications are not widely adopted. Hematopoietic stem cells can be collected either from adult bone marrow or from umbilical cord blood at birth.
Mesenchymal Stem Cells (Tissue-Derived Stem Cells) Mesenchymal stem cells have greater self-renewal and differentiation capacity than hematopoietic stem cells, enabling a broader range of potential applications. These stem cells can be collected from adult adipose (fat) tissue or from umbilical cord tissue at birth. However, collecting tissue-derived stem cells from adipose tissue is more complex, as only certain stem cell banks can process and store this type of tissue, such as MEDEZE.

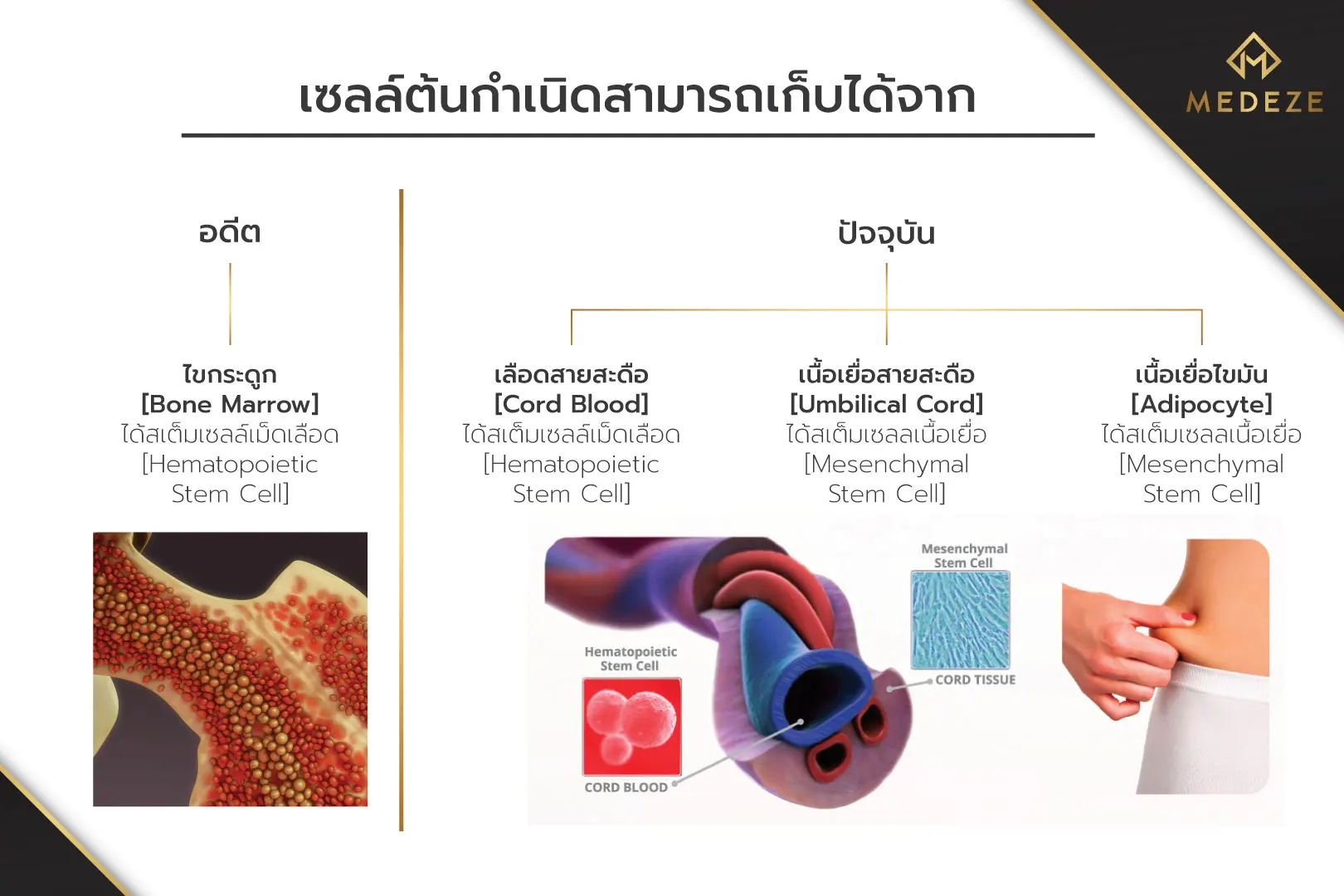
Alternatively, stem cells can be categorized by the source from which they are collected. This classification includes two main groups: stem cells collected from newborns at birth (hematopoietic stem cells from cord blood and mesenchymal stem cells from umbilical cord tissue) and stem cells collected from adults (hematopoietic stem cells from bone marrow and mesenchymal stem cells from adipose tissue).
Advantages of Collecting Stem Cells at Birth
Stem cells collected from different sources each have their own advantages and limitations. Collecting stem cells at birth involves additional costs for storage and maintenance; however, it offers several advantages compared with collecting stem cells later in life.
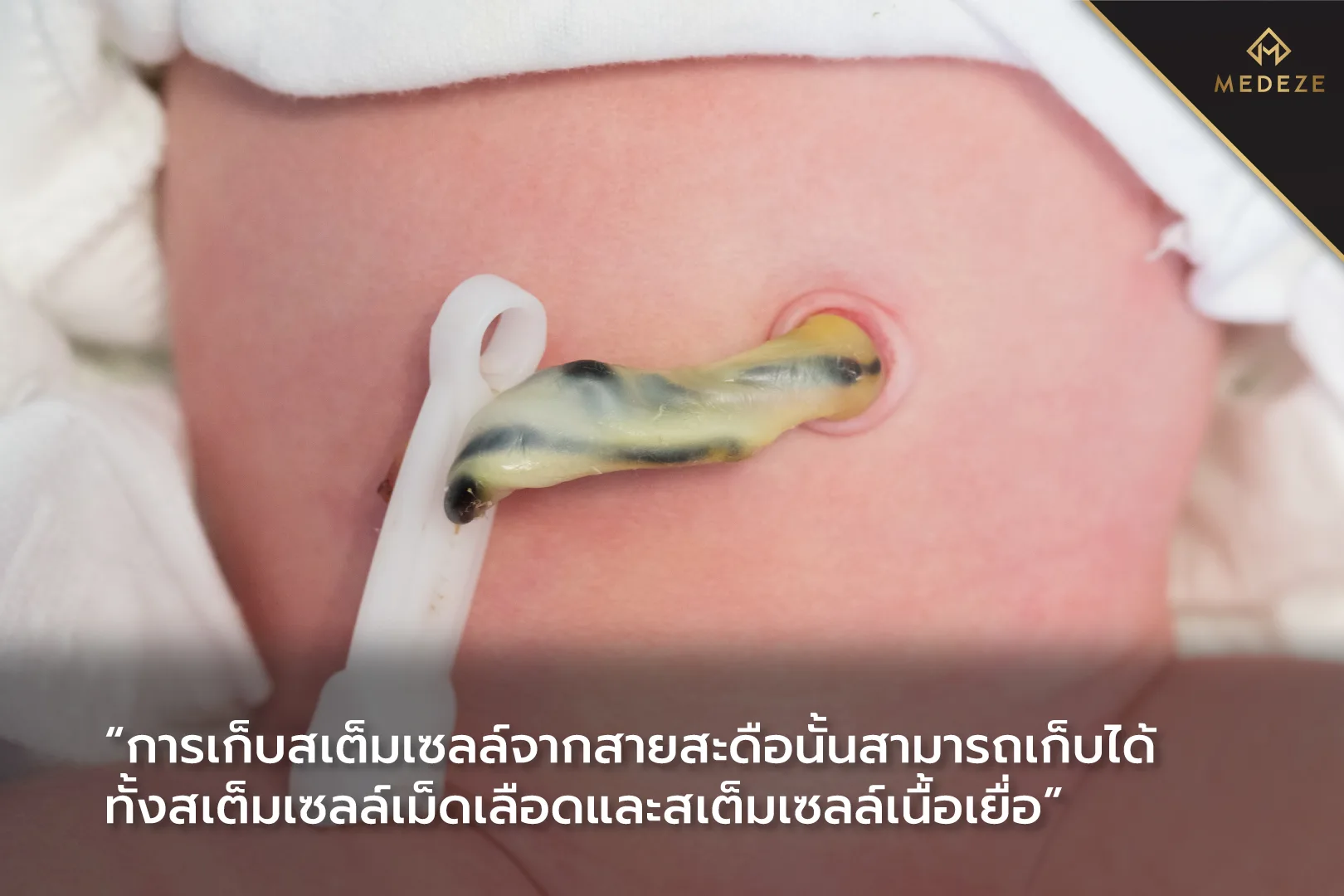
In adults, mesenchymal tissue stem cells are typically obtained by harvesting adipose (fat) tissue from areas such as the abdomen, upper arms, thighs, or hips. Although this procedure is generally safe and commonly performed, it requires additional costs. Alternatively, hematopoietic stem cells must be collected through bone marrow aspiration, which is relatively painful and must be performed in a sterile operating environment. In contrast, umbilical cord tissue and cord blood stem cells in newborns are collected from the umbilical cord or placenta after separation from the infant. Under normal circumstances, the placenta and umbilical cord are naturally expelled and discarded after birth. Therefore, collecting stem cells from newborns does not cause any pain or discomfort to the infant.
Although current clinical applications of stem cells do not differ significantly by source, stem cells derived from umbilical cord tissue have a much higher capacity for cell division and self-renewal. This provides greater potential for novel therapeutic approaches in the future. [4]
Umbilical cord stem cells have not been exposed to external contaminants, such as chemicals or radiation, maintaining optimal cellular integrity. This is consistent with findings from multiple studies reporting that the regenerative potential of stem cells declines with increasing age at the time of collection. [5]
In terms of clinical use, hematopoietic stem cells—regardless of whether they are collected from adult bone marrow or neonatal cord blood—can differentiate only into red blood cells, white blood cells, and platelets. As a result, their applications are mainly limited to hematological diseases.[3]
Tissue-derived stem cells, on the other hand, have a broader differentiation capacity. They can develop into various cell types, such as cartilage, cardiac, and liver cells, enabling a broader range of clinical applications. Due to differences in stem cell types and their biological potential, stem cell collection should be carefully planned based on the intended therapeutic use to achieve maximum effectiveness.
References
1) Nair V, Talwar P, Kumar S, Chatterjee T. Umbilical cord blood transplantation and banking. Pregnancy medicine. 1st ed. Delhi: Jaypee Brothers Medical Publishers (P) Ltd. 2015:197-215.
2) Mayo Clinic Staff. Stem cells: What they are and what they do. [Online]. June 2019. Available at: https://www.mayoclinic.org/tests-procedures/bone-marrow-transplant/in-depth/stem-cells/art-20048117. [August 2021]
3) Kanis Sa-ngiamsuntorn, Ph.D. Stem Cell; Progenitor Cell Part 2: Get to know iPS cells?. [Online]. 2014. Available at: https://pharmacy.mahidol.ac.th/th/knowledge/article/202/สเต็มเซลล์-StemCell-เซลล์ต้นกำเนิด-ตอนที่2-ไอพีเอส/. [August 2021]
4) Mayani H. Biological differences between neonatal and adult human hematopoietic stem/progenitor cells. Stem cells and development. 2010 Mar 1;19(3):285-98.
5) Harris DT. Stem cell banking for regenerative and personalized medicine. Biomedicines. 2014 Mar;2(1):50-79.
Search Articles
Latest Articles
สายสะดือทารกแรกเกิด แหล่งรวมสเต็มเซลล์ ในการรักษาโรคและฟื้นฟูสุขภาพ
What are Mesenchymal Stem Cells (MSCs)? Exploring Their Benefits and Potential
What is Adipose Tissue? Can Fat Tissue Really Help with Anti-Aging?
Understanding Modern Innovation: NK Cells in Eliminating Cancer Cells and Virus-Infected Cells
What are NK Cells? The Immune Cells that Combat Viruses and Cancer Cell
